An Inside Look: The Intricate Tapestry of UK’s Healthcare System
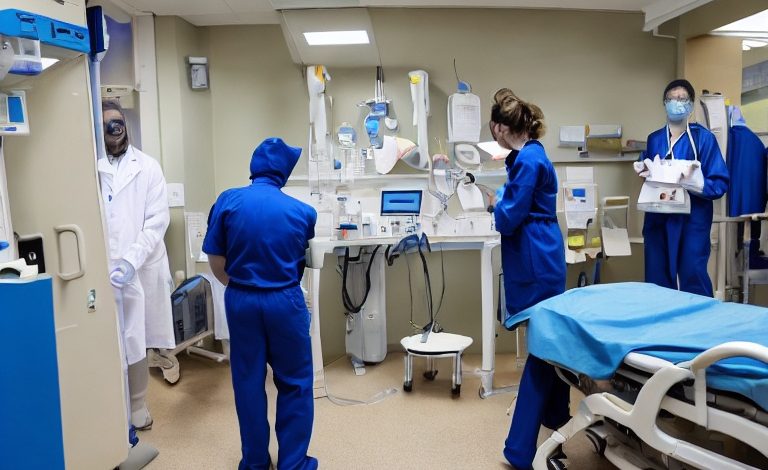
Journey through the winding labyrinth that constitutes the UK’s healthcare system, a complex weave of public and private services, financed by taxation, insurance, and out-of-pocket contributions. As colourful, beautiful, and intricate as a medieval tapestry, it is a diverse melange of elements that underpin the health and wellbeing of British society. Join us as we unravel the delicate threads interlacing prevention, diagnosis, treatment, care, and research; dexterously woven together and unwavering in its aim of providing comprehensive, universal healthcare that leaves no one behind. This intimate exploration will help shed light on this gem of British society, leading you through the triumphs, trials, and tribulations of this fascinating tapestry that is the UK’s healthcare system. It promises to be an enlightening excursion, laden with understanding and insight, so jump aboard and venture with us below the surface.

Decoding the Underpinnings of the UK Healthcare System
The UK’s healthcare system, known as the National Health Service (NHS), is a multi-layered tapestry woven with a series of well-detailed mechanisms, policies, and resources. As one of the world’s largest publicly funded health services, the NHS offers most services free at the point of use, ensuring equitable access to healthcare for all UK residents. This egalitarian principle is at the crux of the NHS and sets it apart from many other healthcare systems.
The structure of the NHS is split into distinct components, each with its unique roles and responsibilities. NHS England and NHS Improvement are responsible for providing strategic leadership for England’s health system. They oversee commissioning, or the planning and purchasing of services, from primary and community care to hospital care. Public Health England is the watchdog for the nation’s health and wellbeing, responsible for disease control and health promotion. The Care Quality Commission serves as the independent regulator for all health and social care services, ensuring standards of care are upheld.
-
- NHS Clinical Commissioning Groups (CCGs): These are the bodies responsible for the planning and commissioning of healthcare services in their local area.
-
- NHS Foundation Trusts and NHS Trusts: These organizations supply ambulance services, hospital care, mental health services, and community health services.
-
- NHS Digital: This body handles information and technology for the NHS, implementing systems and setting standards to ensure that information is managed effectively and consistently.
| Organisation | Role |
|---|---|
| NHS England and NHS Improvement | Strategic Leadership |
| Public Health England | Disease Control and Health Promotion |
| The Care Quality Commission | Ensuring Standards of Care |
It’s essential to understand these backbones of the NHS to decode how the UK’s healthcare system operates effectively and remains accessible for everyone, regardless of their financial status. With its complexity and vastness, the UK’s healthcare system indeed is nothing short of an intricate tapestry.

The NHS: Architect of the UK’s Healthcare Tapestry
In the heart of the UK’s health and wellbeing infrastructure stands the NHS (National Health Service), a beacon of public service since its birth in 1948. Providing care ‘from cradle to grave’ as its founder, Aneurin Bevan, succinctly put it, the NHS is the institution that weaves the complex threads of the UK’s healthcare system. It is the primary provider of healthcare services in the country and caters to a population of over 60 million, accomplishing this massive feat via a large network of hospitals, clinics, and other health facilities sprawled across the nation.
Let’s try to unravel this grand tapestry woven by the NHS. Their services range from routine screenings, treatments for long-term conditions, transplants, emergency treatment, and end-of-life care. Here’s a snapshot of services:
-
- General Practitioners (GPs): Usually the first point of contact, GPs manage a broad variety of health conditions.
-
- Hospitals: They provide secondary care ranging from accident and emergency services to elective surgery and specialist clinics.
-
- Pharmaceutical Services: Patient medication needs are addressed here, in close conjunction with GPs and hospitals.
Furthermore, there is a maze of NHS trusts responsible for different aspects of care. Such includes Ambulance Trusts, Mental Health Trusts, and Acute Trusts.
| Type of NHS Trust | Role |
|---|---|
| Ambulance Trusts | Provide emergency access to healthcare – their services are vital in directing patients to the correct area of care. |
| Mental Health Trusts | Offer specialist care and treatment to support people with mental health issues. |
| Acute Trusts | Primarily operate hospitals, including Emergency Department services, they handle the majority of hospital admissions. |
Each strand meticulously intertwined by the NHS crafts a system that stands as one of the finest examples of free healthcare in the world. This tapestry, albeit complex, is held together by the principle of universal care - free at the point of use, based on need and not the ability to pay.
The Dance of the Public and Private Sectors in UK Healthcare
The realm of healthcare in the UK is a complex interplay of several players, each with their unique roles and responsibilities. Central to this are two key participants: the public and the private sectors. The public sector, primarily represented by the National Health Service (NHS), manages the lion’s share of healthcare services and facilities in the country. It’s their role to ensure the majority of UK residents have access to critical healthcare facilities without being financially burdened. Conversely, the private sector, consisting of private healthcare organizations, consultants, and pharmaceutical companies, plays a complementary role, filling gaps in the NHS’s coverage and offering additional services that may not be readily available in the public sector.
In harmony with each other, these two sectors form a dynamic dance, balancing and compensating for each other’s weaknesses. For example, in scenarios where NHS’s resources are limited or overstrained, patients may opt for private healthcare options to receive faster treatment. Additionally, private sector companies invest heavily in innovative drug discovery and medical technologies, leading to advancements that propagate through the entire system. It’s to note, however, that the balance of this dance isn’t always perfect, leading to challenges and debates on the overall efficiency and fairness of the UK’s healthcare system.
| Key Player | Primary Role |
|---|---|
| NHS | Main provider of healthcare services, ensuring widespread access |
| Private Sector | Supplementation of public services, innovations and faster treatments |
This intricate interplay of public and private sector forms a unique tapestry that’s constantly evolving, leaving room for continued analysis and potential reforms. It’s clear to see that the dance of these two sectors is at the heart of the UK’s healthcare system, ensuring access, encouraging innovation, tackling challenges, and ultimately, safeguarding the health of the nation.

Championing Improvement: In-depth Recommendations for UK’s Health Sector
The complex network of the United Kingdom’s healthcare system is a vast, multidimensional tapestry that integrates both public and private provision. Its cornerstone is the maverick National Health Service (NHS), which provides healthcare services that are largely free at the point of use. Yet, with growing demands, escalating costs and ever-evolving medical technology, the system faces significant challenges which need impactful actions for sustainable enhancement.
Developing a Patient-Centered Model. Understanding that the patient is the center of the healthcare ecosystem is pivotal. A seamless, integrated approach can not only improve patient outcomes but also reduce the burden on the system. This can be achieved by:
-
- Promoting self-care and preventative measures: Empowering individuals to take control of their health could reduce the pressure on services.
-
- Ensuring continuity of care: This involves better coordination between different healthcare providers and ensures patients receive the right care, at the right time, in the right place.
-
- Making services more accessible: Using digital technology to facilitate online consultations and remote monitoring, particularly in rural or hard-to-reach areas.
Investing in Workforce Planning. Without a doubt, the backbone of the UK’s healthcare sector is its workforce. Strategies to cultivate a resilient, competent and diverse workforce include:
-
- Retaining talent: Implement initiatives that encourage staff retention, such as flexible working hours, career development pathways, and well-being programs.
-
- Expanding the skill mix: Enabling allied health professionals to take on expanded roles can ease the burden on physicians and improve service delivery.
-
- Fostering a culture of continuous learning and innovation: Ensure healthcare professionals have access to training and development opportunities that keep them up-to-date with the latest advancements in medical science and technology.
| Recommendations | Potential Impact |
|---|---|
| Develop a patient-centered model | Improvement in patient outcomes and reduced burden on the system |
| Invest in workforce planning | Increased retention, expanded skill mix, and promotion of learning and innovation |
Wrapping Up
In summary, we’ve embarked on a journey through the elegant labyrinth that is the UK’s healthcare system. Pulled back the curtains on its vast, intricate tapestry – woven with the threads of medical excellence, public welfare, economic policies, and social structures. And yet, for every thread unspooled, another waits in the shadows, a testament to the extraordinary complexity and depth of this subject. Each divergence in policy or practice contains countless sub-stories and perspectives, each a vital part of the broader narrative.
The UK’s healthcare system, while not without its challenges and occasional cracks, continues to be a beacon of resilience and adaptability – a personification of its ethos engrained on collective hearts, ‘healthcare, accessible for all.’ It stands tall, preserving Leonardo da Vinci’s poignant sentiment, ‘vitality and beauty are gifts of nature for those who live according to its laws’.
Just as taking apart a tapestry unravel its beauty, a full comprehension of the healthcare system might be beyond reach, and perhaps not even necessary. But appreciating the rich details, deep complexities, and the sheer enormity of this tapestry – that is both, a quest and a reward. Because every thread counts. And as long as these threads pulse with commitment to patient care, the UK’s healthcare tapestry will shimmer with robust health, and continue to be a glorious testament to human endeavor and dedication.
As we draw this discourse to its close, let’s remember – no matter where we step into this labyrinth, no matter which thread we pull from this tapestry, it is all part of a larger whole. A part of a healthcare system that has at its heart, a heartbeat. A tireless, unwavering, resolute heartbeat. One that pulses not in decibels, but in deeds; not in echoes, but in empathy. And therein lies its truest triumph. So here’s to the labyrinthine complexity, and the enduring heartbeat of the UK’s healthcare system.



